Editor’s Note: Earlier this month, Dr. Robyn Gartrell, a Pediatric Hematology/Oncology Fellow here, traveled to National Harbor, MD, for a conference on immunotherapy. Next to precision medicine, immunotherapy is probably the area of research most people ask about. Thanks to Robyn, we can now present this summary of the work being done at Columbia University Medical Center and how it relates to childhood cancer.
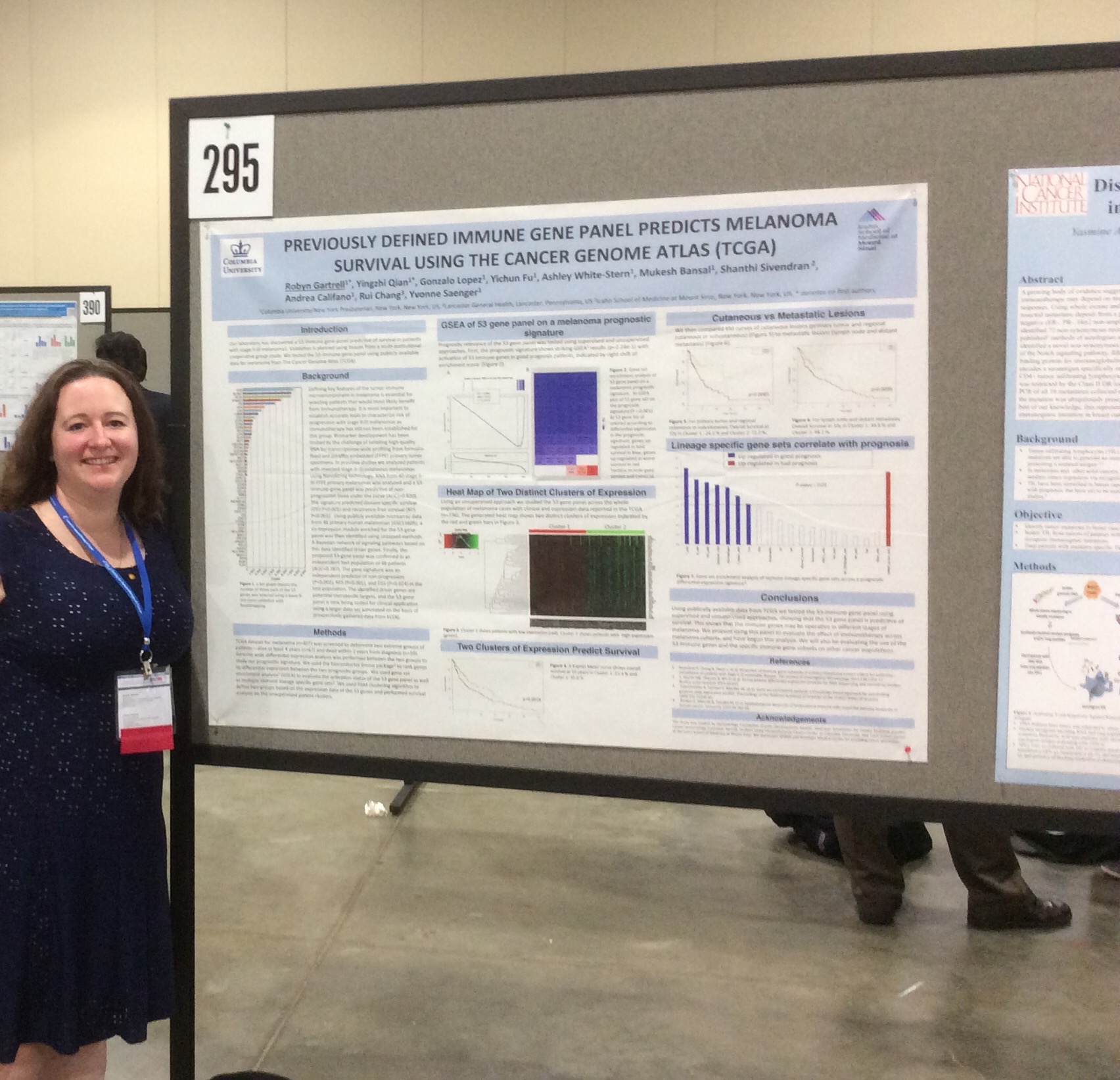
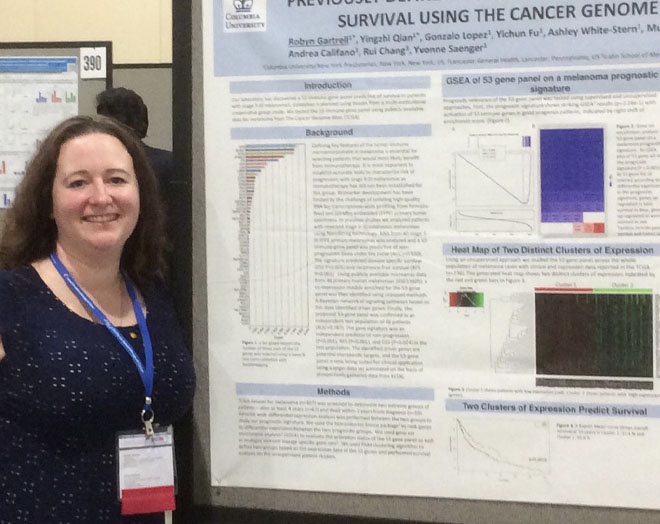
Dr. Robyn Gartrell with her poster at SITC.
The Society for Immunotherapy in Cancer (SITC) conference first met in 1985 when immunotherapy treatment was in its infancy and the only option for immunotherapy was Interleukin 2. As the ability to use the immune system to treat cancer has developed over the last 30 years we are now seeing a large shift in the mindsets of adult oncologists across the world to consider immunotherapy as first line agents to treat some of the sickest patients. This therapy is now offering a cure to previously devastating diseases. Just five years ago only around 200 people were attending SITC conferences and this year there were nearly 2200 people in attendance with 476 posters presented and over 50 oral presentations by the most renowned immuno-oncologists in the world.
As a physician in training I have been fascinated by the immune system in relation to oncology and was grateful to have the opportunity to attend this groundbreaking conference and present a poster. My Primary Investigator, Dr. Yvonne Saenger is an immune-oncologist who works with melanoma. She discovered an immune gene panel that predicts survival in stage II-III melanoma and my presentation involved applying this immune gene panel to The Cancer Genome Atlas (TCGA). This is considered immunogenomics, a very new field in the world of immuno-oncology. We applied the immune gene panel to over 300 patients in the TCGA with melanoma. The immune gene panel was predictive of survival regardless of stage or location of biopsy.
Many people were interested in our findings and the overall impression of our poster was very positive. We also learned that there were other labs doing similar work on other adult cancers. The application of the immune gene panel to TCGA is only a small part of my project as a fellow as I plan to further validate the panel using immunohistochemistry (IHC) of antibodies within the panel on clinical samples collected at Columbia. We will also be applying the immune gene panel to evaluate peripheral blood of patients treated with immunotherapy. Both the IHC and peripheral blood application of the immune gene panel is important as one of the greatest needs in immune-oncology is discovery of biomarkers to predict which patients will benefit from immunotherapy. This was a hot topic at the conference and subject of many presentations.
In its application to pediatric oncology, Immunotherapy has only just begun. SITC included presentations on further success using T-cell therapy in treatment of relapsed childhood leukemia. However, there is much that is still to be done going forward especially in research for solid tumors and neuro-oncology. This work starts in the lab so we can learn when and how to use immunotherapy in children with cancer. My next step is to apply what I have learned about immune-oncology from my work with Dr. Saenger as well as my experience at SITC to further research immune oncology and immune genomics as it applies to pediatric oncology. I hope to be one of the pioneers in this field and SITC was a real spark to my interest. I believe that immunotherapy can be the light at the end of the tunnel for many childhood cancers, especially those that are unresponsive to traditional therapy.
If you are interested in supporting Robyn’s research or any of our other activities, please visit this page.